

MEN’S HEALTH – ISSUES RELATED TO PROSTATE
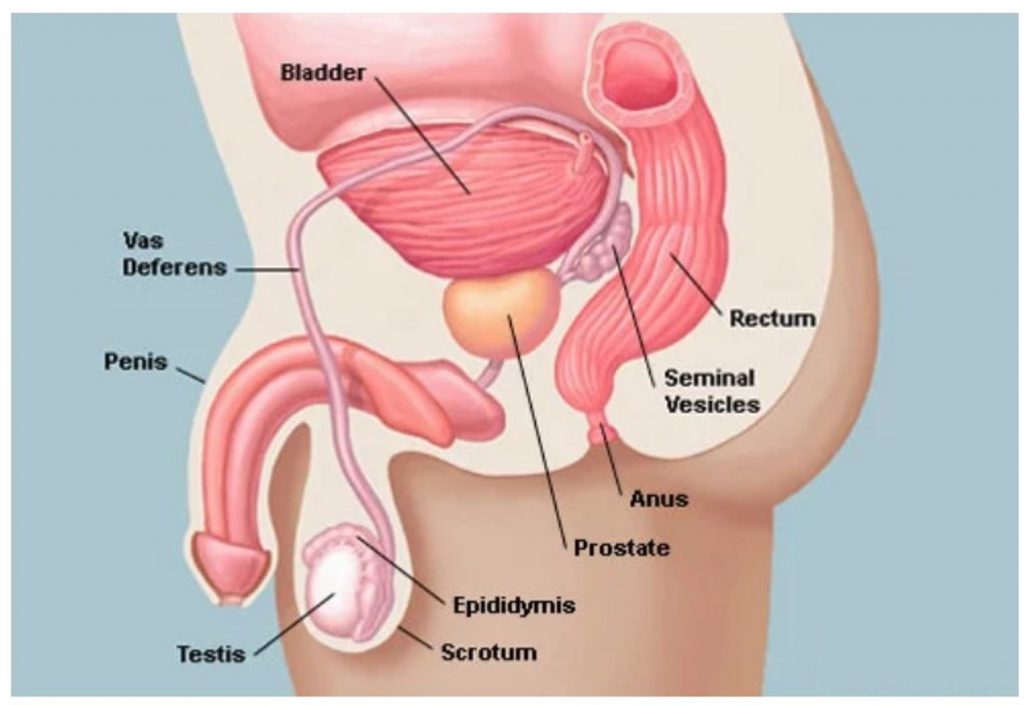
What is prostate?
The prostate is a gland that is a part of the male genitourinary system that wraps around the male urethra near the bladder. The prostate gland has functions which are important to reproduction as well as control of urination. The prostate gland produces prostatic fluid which contains enzymes, proteins, minerals that protect & nourishes sperms. Secretions from prostate gland mixes with fluid from seminal vesicles (present on both sides of prostate) and vas deferens to form semen. Disease processes involving the prostate are common after 50 years of age, although it may start earlier. The prostate grows larger as one ages. In adult young men, a typical prostate is about 3 cm thick and 4 cm wide (about the size of a walnut) and weighs about 20 grams and starts to get larger when men reach their 40’s and early 50’s.The most common problem associated with prostate is due to its enlargement and in a significant number of people this is noncancerous viz benign. This is in medical terms called as Benign Prostatic Hyperplasia (BPH).
Common prostate problems in men –
- Benign prostatic hyperplasia (BPH)
- Prostate cancer
- Acute and chronic bacterial prostatitis
- Chronic prostatitis (non-bacterial)
- Tuberculosis of prostate (Uncommon)
Symptoms due to prostate diseasesEnlargement of the prostate gland can cause symptoms like – Difficulty in starting urination, slow urine stream, straining during urination, dribbling of urine after urination, pain or burning sensation during urination, feeling of incomplete evacuation of urine, frequent urination, inability to postpone urination viz urinary urgency which may be associated with leakage of urine before reaching the toilet (urge incontinence), frequent urination in the night (nocturia) which can significantly affect the quality of sleep, blood in the semen or urine etc.
In addition to the above symptoms, prostatic infections can cause frequent pain or stiffness in the lower back, hips, pelvic or rectal area, or the upper thighs, painful ejaculation, lower abdominal or perineal pain and occasionally fever if it is an acute infection. These symptoms my occur if there is pus collection in the prostate as well (prostatic abscess).
Prostate cancer also produces similar symptoms as BPH and so it is impossible to differentiate between the two based on symptoms alone. Occasionally the initial symptoms may be ignored and this can cause dissemination of cancer over a period of time causing symptoms related to disseminated cancer like bone pain, back pain etc. Back bone is a common site of dissemination of prostate cancer and so back pain in someone with prostate cancer needs prompt evaluation and treatment.
There is considerable overlap of symptoms of conditions like urethral stricture, bladder neck stenosis, neurologic issues causing voiding disability etc with symptoms due to prostatic enlargement. Hence it is imperative that patients with urinary symptoms be evaluated by a urologist to identify the cause correctly.
Diagnosis of prostate problems
To diagnose the cause of the prostate problem, after evaluation of the symptoms of the patient, the doctor will do a digital rectal examination, and take bacterial cultures if infection is suspected. Rectal examination is performed by inserting a gloved and lubricated finger through the anal opening. This would help in assessing the size and condition of prostate and may give a clue to the diagnosis of prostate cancer. However in early stages of prostate cancer, when there is only a small focus of malignancy, rectal examination may not be able to detect prostate cancer. Additional information gathered with a rectal examination would include the anal tone and neural reflexes which are useful in assessing neurological issues causing voiding disability.
In addition to clinical examination, the urologist performs a few labs tests and ultra sound scan to assess the prostate, bladder and kidneys. Another common test performed is a Uroflowmetry to assess the strength of urine stream. Tests like Trans rectal ultra sound scan, MRI scan, Gallium PSMA PET scan, Bone scan, Urodynamics etc are done in special situations.
PSA test
PSA (Prostate Specific Antigen) is a substance secreted predominantly by the prostate and the level of this in blood can be quantified by blood tests. PSA levels in serum becomes elevated in several disease processes involving prostate like infections, prostatic hyperplasia, after catheterisation etc and most importantly prostate cancer. Hence this test is used as a screening tool to detect prostate cancer. However, the caveat is that the level of PSA in blood can be reasonably high in certain non-cancerous conditions also and hence the interpretation of abnormal levels of PSA in blood has to be made with caution and this certainly needs expert evaluation by a urologist to make a correct diagnosis. The levels of PSA are < 4 ng/mL in most healthy men. As PSA levels go up, the chances of having prostate cancer increase. However, a PSA level of <4 does not always guarantee exclusion of cancer; about 15% of men will still have prostate cancer on biopsy. There is about 1 in 4 chance of having prostate cancer in men with PSA between 4 and 10 ng/ml and if PSA is >10, the chance increases to 50%.The PSA level in blood is also an important tool for monitoring the recurrence and progression of cancer in patients who are treated for prostate cancer.
When should someone seek medical attention to evaluate prostate issues?
Diseases afflicting prostate are very common beginning the fifth decade of life. It is needless to say that detection of prostate cancer at an early stage is of vital importance to cure the disease. Any person experiencing the symptoms mentioned above that are related to prostate problems should seek medical attention. Screening for prostate cancer is available with PSA test. It is recommended that all men have a blood test to assess blood levels of PSA at least once a year, starting from fifty years of age. This can be started as early as forty five years in persons who have a family history of prostate cancer. It is advisable to have a evaluation by a urologist if there is an abnormal level of PSA and if there are any symptoms related to urination.
Treatment of prostatic ailments
Treatment of prostatic diseases is dictated by the cause which is identified after evaluation. The most common affliction of prostate is prostatic enlargement due to benign prostatic hyperplasia (BPH). Patients with BPH and mild symptoms who are not significantly bothered are treated with life style modifications alone and may not need medicines. For others who require treatment, several drugs are available which effectively control symptoms. Treatment with medicines may have to be continued for prolonged periods. For patients who are troubled by severe symptoms who do not respond to medical treatment and those who have complications associated with BPH, would require surgery. There are potential complications that are associated with BPH if left untreated – recurrent urinary infection, urinary retention, bladder stones, impairment of kidney function etc. Another common indication for surgery is acute urinary retention where in the person may not be able to pass urine and would urgently require insertion of urinary catheter to drain urine.
Prostatic infections would require prolonged treatment with antibiotics for clearance of infection and pus collections inside prostate would in addition require drainage of pus. Diseases like chronic prostatitis (non-bacterial) also requires prolonged treatment. Various life style changes also would help such patients.
Surgery for BPH
Most patients with BPH can be operated endourologically without creating any external wound. The most commonly performed operation is TURP (Trans urethral resection of prostate). This involves passage of a special instrument through the urine passage (urethra) to access the prostate and the prostate is removed in small pieces. Open surgery is reserved for patients with a large sized prostate. Other advancements in the surgical treatment for BPH is the use of lasers for prostate surgery. Surgical techniques like Laser enucleation of prostate and Laser vaporization of prostate is now available. All these minimally invasive surgical options for prostate surgery aids in rapid recovery of patients back to normal life without having the requirement of bearing a surgical scar.
Prostate cancer
Prostate cancer is most common among African-American men. Prostate is the second leading site of cancer among males in large Indian cities like Delhi, Kolkatta, Pune and Thiruvananthapuram, third leading site of cancer in cities like Bangalore and Mumbai and it is among the top ten leading sites of cancers in the rest of the population based cancer registries (PBCRs) of India. If someone’s father or brother has had prostate cancer, they are more likely to have it, too. Eating high-fat food with few fruits and vegetables and a diet rich in calcium may raise the risk of developing prostate cancer.
A definitive diagnosis of prostate cancer can be made only with biopsy from the prostate. Biopsy from the prostate is taken as a needle biopsy through transrectal route. A trans rectal ultrasound is useful in guiding biopsy. The biopsy is sent to the pathologist who examines it to look for any cancer cells and also to grade the cancer for finally assessing the severity of the disease.
Once the diagnosis of prostate cancer is made, the treatment decision is made taking into consideration several factors. The age at diagnosis, stage of cancer, general condition of the patient and peculiarities in the pathological report (tumour grade) are important factors in making a decision as to how to treat prostate cancer. In general, a malignant process confined to the prostate without any spread outside the prostate is treated by surgery to remove the prostate (radical prostatectomy) or by radiotherapy (radical radiotherapy). Advancements in surgery like robotic surgery has made surgery for prostate cancer safer with lesser chances of complications. The most common sites of spread of prostate cancer are lymph nodes and bones. Prostate cancer which has spread to bones and significant number of lymph nodes are treated with hormonal therapy. Prostate cancer has a unique nature – it requires the hormone testosterone for growth. Testosterone is mainly produced from the male gonads (testes) and a small amount is produced from adrenal glands. Hormone therapy in the treatment of prostate cancer aims at eliminating testosterone in the body – either by a surgery to remove testes (orchidectomy) or by administering medicines to suppress testosterone production from testes. In addition, testosterone from adrenal glands are also blocked with medicines. There are a number of advancements in the treatment of advanced prostate cancer. These include medicines that are used as chemotherapeutic agents as well as newer hormone blocking agents. Another advancement is the use of radiopharmaceuticals in the treatment of advanced prostate cancer – Lutitium PSMA therapy, Actinium PSMA therapy. The selection of treatment is made judiciously be a team of doctors including urologist, medical and radiation oncologist and nuclear medicine specialist. There are other treatment modalities which utilize the body’s immune system to treat advanced prostate cancer – such a treatment (Sipuleucel-T) is not widely available in our country.
Prevention of prostatic diseases
Life style modifications have been seen to reduce the risk of developing diseases related to prostate. Although the occurrence of BPH cannot be prevented completely, early recognition of symptoms and timely treatment can reduce complications associated with it. It is advisable to have the following preventive measures for a healthy prostate –
Drink more water: Staying properly hydrated is essential for maintaining good prostate health. Dehydration and urinary tract infections are risk factors for prostatitis and can worsen symptoms.
Practice good hygiene: Keeping the penis and surrounding area clean can reduce the risk of infection.
Reduce caffeine and alcohol intake: Caffeinated beverage and alcohol can irritate the urinary bladder and prostate and worsen the symptoms of prostatitis. Symptoms like frequency and nocturia (urinating more in night) are also worsened by caffeine and alcohol.
Practice safe and healthy sex: Certain sexually transmitted diseases can cause bacterial prostatitis. Practicing safe sex, by using a condom, will reduce the risk for prostatitis. There are studies which state that having more than 21 ejaculations per month during early adult life offer some protection against prostate cancer later in life.
Exercise: Regular physical activity has an impact on the prevention of both prostatitis and inflammation.
Choose a low-fat diet : Foods that contain fats include meats, nuts, oils and dairy products, such as milk and cheese. High fat diet has been seen to be associated with increased risk of prostate cancer.
Reduce consumption of dairy products : In studies, men who ate higher amounts of dairy products such as milk, cheese and yogurt each day had higher risk of prostate cancer. But study results have been mixed, and the risk associated with dairy products is thought to be small.
Consume more fruits and vegetables: Fruits and vegetables contain high levels of antioxidants, vitamins and other nutrient that will help in fighting infections and inflammation. This would also leave lesser room for consumption of fatty food which is unhealthy.
Maintain a healthy weight: Being overweight is detrimental to overall prostate health.














